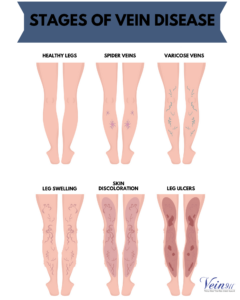
Unfortunately, vein disease is primarily genetic and you cannot pick your parents. There is no evidence that any drug, vitamin or nutraceutical will slow the progression of your vein disease. However, you can take some conservative measures to slow the progression of your vein disease. However, the below lifestyle changes can help with vein related symptoms:
- Walk, exercise or swim! Remember, we have “3” hearts! The heart we all know about in our chest and the two we forget about in each of our calf muscles called the “calf muscle pump.” Contracting your calf muscle keeps your blood and lymph fluid from pooling in your legs which can lead to damage to your veins and unwanted symptoms.
- Sit at the proper height! We often sit too high and put pressure on the back of our thighs. We should sit on our “butt bones,” not our thighs. Prolonged pressure on the back of your thighs compresses venous blood outflow and lymph fluid outflow, which may cause or worsen leg, ankle, and foot swelling.
- Wear graduated compression hose! A quality pair of measured and fitted, medical-grade “graduated” compression hose are a wonderful thing. Ask your Vein Care Specialist for details.
- Maintain an ideal body weight! An ideal body weight improves your mobility, allowing more exercise, which prevents blood pooling in your legs